Of all the experts I’ve talked to about the coronavirus this week, Dr. Maria Raven is by far the most cool, calm, and collected. Maybe it shouldn’t come as a surprise: It’s basically a part of her job description as the chief of emergency medicine at UCSF Medical Center, the Bay Area’s largest hospital. Now, the celebrated medical institution is smack dab in the middle of a coronavirus hot spot.
As of Monday afternoon, nearly 300 cases of the infection had been reported in six Bay Area counties, leading officials to call on more than 6 million residents in the counties to shelter in place. San Francisco is suspended in a sense of something like impending doom: As ProPublica recently noted, if the city follows what one set of Harvard researchers considers a “moderate” infection trajectory, more than 100,000 residents would require hospitalization. If those 100,000 cases occurred over a 12-month period—a timeline that is itself a moderate estimate—the city would need “three times the number of available hospital beds and ICU beds it has,” ProPublica reported.

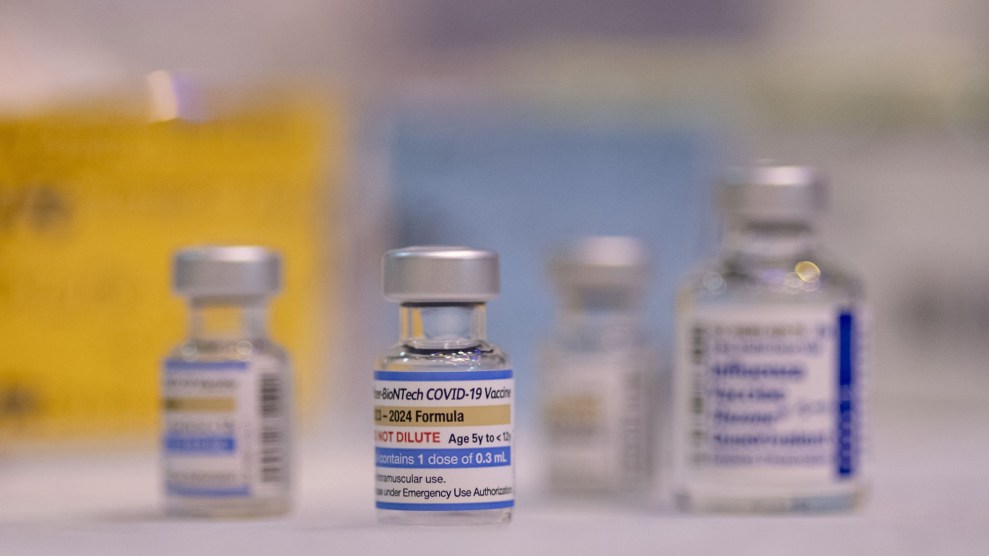
An accelerated care unit at UCSF, where patients with respiratory symptoms are being triaged.
Noah Berger / UCSF
UCSF has a mere 600 beds at its main campus. Like many hospitals around the country, it has mobilized in recent weeks to prepare for an influx of new patients. “We’ve got all these things in place for if we see a huge surge,” Raven told me on Monday. “Everyone’s waiting with bated breath: like, when is this going to hit?” The hospital canceled elective surgeries to free up manpower, bed space, and, supplies, and it set up “COVID wards” for patients admitted to the hospital with coronavirus. As of Monday, security guards are posted outside the hospital to screen every person as they walk in, asking questions about respiratory symptoms, fevers, and “high-risk contact” with anyone with coronavirus.
Last week, the hospital erected two military-grade tent structures in the parking lot to triage incoming patients with respiratory symptoms: one for less ill, “treat-and-release” patients, the other for more serious cases that may necessitate being admitted to the hospital. It includes things you’d associate with an emergency room: gurneys, X-ray and electrocardiogram machines, computers and wifi. Together, the tents, called accelerated care units, can hold roughly 25 patients at a time. Dozens of patients are already are being treated in the structures each day.
UCSF is already rationing protective equipment: employees are now reusing masks, gowns, face shields, and the helmet-like gear, called PAPRs, that aren’t visibly soiled, disinfecting them and storing them in big Ziploc bags labeled with their names. (The Centers for Disease Control and Prevention has okayed reusing protective masks when supplies are running low.) “We don’t want to burn through our [protective equipment] and then not have enough,” Raven explains. For now, the hospital has a two-week supply of most of the gear.
Some clinicians have tested positive for the coronavirus in recent days. A UCSF spokesperson didn’t specify how many, but said, “We have not confirmed any that have been infected while caring for patients. Given the broad community transmission right now, as well as their personal histories, there is reason to believe that all were infected in the community.”
Raven is acutely concerned with protecting the wellbeing of the many health care providers—physicians, nurses, and more—who staff the emergency room. Those with fevers or any hint of sore throat or cough are instructed to stay home. Should more colleagues fall ill, or if there is a big jump in patients, the hospital is staffing more nurses than usual and putting more physicians on backup call. And if need be, providers may be asked to practice outside their speciality; surgeons, for example, could be called on to provide emergency room care.
“It feels like nothing else I’ve ever been through before, either as a member of society or as a physician,” Raven said. “What we’re seeing in Italy and the other parts of the US are really, really frightening people.” She is hopeful that recent efforts throughout the Bay Area to stay home and socially distance will help. For now, it’s too soon to tell: “We’ll know a lot more in the next week,” she said.
At the end of our conversation, I asked how Raven herself was doing. She paused. “I don’t think it hit me until this weekend that it’s a lot. It’s a lot of—it’s a heavy prospect.”