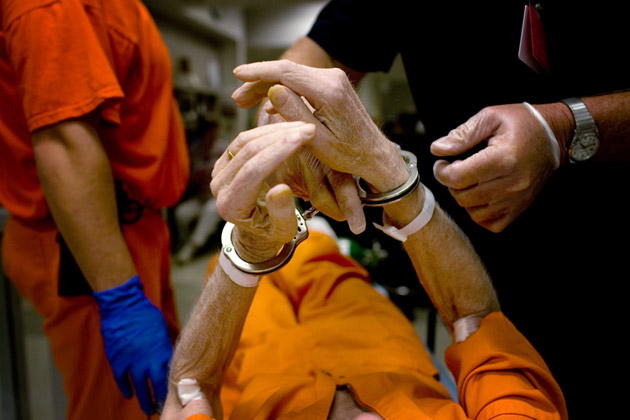
A Kentucky inmate is admitted to the hospital. Click here to see more photos from a prison nursing unit.Tim Gruber
Editor’s note: This article was supported by a MetLife Foundation Journalists in Aging Fellowship, a collaboration of New America Media and the Gerontological Society of America.
William “Lefty” Gilday had been in prison 40 years when the dementia began to set in. At 82, he was already suffering from advanced Parkinson’s disease and a host of other ailments, and his friends at MCI Shirley, a medium security prison in Massachusetts, tried to take care of him as best they could. Most of them were aging lifers like Lefty, facing the prospect of one day dying behind bars themselves, so they formed an ad hoc hospice team in their crowded ward. They bought special food from the commissary, heated it in an ancient microwave, and fed it to their friend. They helped him to the toilet and cleaned him up. Joe Labriola, 64, tried to see that Lefty got a little sunshine every day, wheeling his chair out into the yard and sitting with his arm around him to keep him from falling out.
But Lefty, who was serving life without parole for killing a police officer during a failed bank heist in 1970, slipped ever deeper into dementia. One day he threw an empty milk carton at a guard and was placed in a “medical bubble,” a kind of solitary confinement unit with a glass window that enables health care staffers to keep an eye on the prisoner. His friends were denied entrance, but Joe managed to slip in one day. He recalls an overpowering stench of piss and shit and a stack of unopened food containers—Lefty explained that he couldn’t open the tabs. Joe also noticed that the nurses in the adjoining observation room had blocked the glass with manila folders so they wouldn’t have to look at the old man.
Lefty had been popular among the prisoners, though. A minor-league ballplayer turned 1960s radical—his southpaw, not his politics, earned him the nickname—he was the subject of one of the most infamous manhunts in Massachusetts history. He had already been in and out of prison several times on robbery offenses when he fell in with a group of Brandeis University students who decided that stealing guns and money could help them foment a black revolution. They held up a bank in 1970, and when Boston police responded, guns drawn, a patrolman named Walter Schroeder was shot dead. Lefty claimed that he never meant to shoot the guy—that it was a warning round that ricocheted—but the jury didn’t buy it, and he was convicted of first-degree murder and sentenced to death. (The students got no more than seven years.)
In 1972, after the Supreme Court briefly banned capital punishment, Lefty became a lifer. Over time, he also became a jailhouse lawyer—a inmate paralegal who puts together legal cases for fellow prisoners—settling disputes and eventually gaining a rep as something of an elder statesman. When Lefty died last September, his friends were denied permission to hold a memorial service in the prison chapel, so they ended up holding it in a classroom. The service culminated in some 80 men sailing paper planes into the air as a tribute. “We loved the old man,” Joe Labriola wrote me in a letter.
Lefty Gilday was no ordinary inmate, but in one regard he typified a growing segment of America’s inmate population—geriatric prisoners. The United States leads the world in incarceration, with more than 2.2 million people in its prisons and jails, and the graying of this population is shaping up to be a crisis with moral, practical, and economic implications for cash-strapped governments. In recent years, a growing number of advocates—and even a handful of corrections officials and politicians—have dared to suggest that we consider setting some of these old-timers free.
As of 2010, state and federal prisons housed more than 26,000 inmates 65 and older and nearly five times that number 55 and up, according to a recent Human Rights Watch report. (Both numbers are significant, since long-term incarceration is said to add 10 years to a person’s physical age; in prison, 55 is old.) From 1995 to 2010, as America’s prison population grew 42 percent, the number of inmates over 55 grew at nearly seven times that rate. Today, roughly 1 in 12 state and federal prison inmates is 55 or older.
The trend is worsening. A new report from the American Civil Liberties Union estimates that, by 2030, the over-55 group will number more than 400,000—about a third of the overall prison population. (See chart.) “It’s huge,” says Bob Hood, the former warden of the mammoth federal correctional complex in Florence, Colorado. “We’re behind the eight-ball on this.”
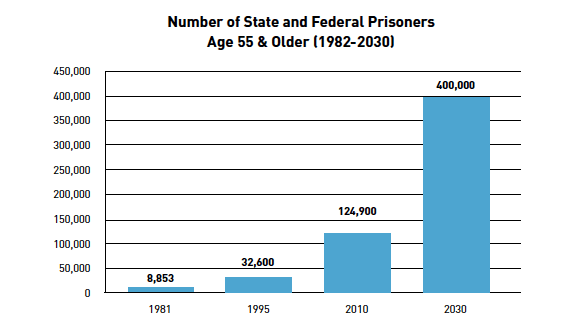 From ACLU report: “At America’s Expense: The Mass Incarceration of the Elderly
From ACLU report: “At America’s Expense: The Mass Incarceration of the Elderly
The boom in geriatric prisoners is the inevitable result of legislation from the tough-on-crime 1980s and 1990s, which extended sentences and slashed parole opportunities, both dramatically so. According to a June report by the Pew Center on the States, drug offenders released in 2009 had spent 36 percent longer behind bars, on average, than those released in 1990. One in ten state prisoners nowadays is a lifer, and about the same proportion of federal prisoners over 50 are serving 30 to life. In short, more than 100,000 prisoners are currently destined to die in prison, and far more will remain there well into their 60s and 70s. Many of these men—as most of them are men—were never violent criminals, even in their youth. In Texas, for example, 65 percent of the older prisoners are in for nonviolent acts such as drug possession and property crimes.
Keeping thousands of old men locked away might make sense to die-hards seeking maximum retribution or politicians seeking political cover, but it has little effect on public safety. By age 50, people are far less likely to commit serious crimes. “Arrest rates drop to 2 percent,” explains Hood, the retired federal warden. “They are almost nil at the age of 65.” The arrest rate for 16-to-19-year-olds, by contrast, runs around 12 percent.
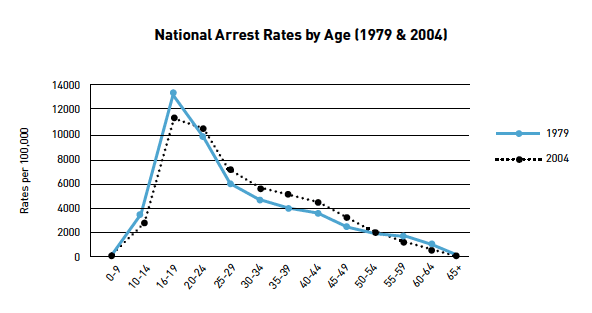 From ACLU report: “At America’s Expense: The Mass Incarceration of the ElderlyOnce released, therefore, the vast majority of the older prisoners never return. Data from New York state, for example, tracked 469 inmates who were originally sentenced for violent crimes and were later released as senior citizens—over a 13-year period, just 8 of those former inmates went back to prison, and only 1 went back for a violent offense. “The mass incarceration of the elderly is an example of our criminal justice system at its most heartless and its most irrational,” says David Fathi, director of the ACLU’s National Prison Project. “Most such prisoners are long past their crime-prone years and pose little to no public safety risk.”
From ACLU report: “At America’s Expense: The Mass Incarceration of the ElderlyOnce released, therefore, the vast majority of the older prisoners never return. Data from New York state, for example, tracked 469 inmates who were originally sentenced for violent crimes and were later released as senior citizens—over a 13-year period, just 8 of those former inmates went back to prison, and only 1 went back for a violent offense. “The mass incarceration of the elderly is an example of our criminal justice system at its most heartless and its most irrational,” says David Fathi, director of the ACLU’s National Prison Project. “Most such prisoners are long past their crime-prone years and pose little to no public safety risk.”
Beyond any questions of efficacy or mercy lies the looming issue of the price tag. According to the ACLU, caring for aging prisoners costs American taxpayers some $16 billion annually. We shell out roughly $68,000 a year for each inmate over 50, twice what it costs to keep a younger person locked up. And the older the inmate, the greater the cost. “I’ve had inmates where a total cost of $100,000 a year is on the low side,” Hood says.
Even when you factor in post-incarceration expenses—for parole, housing, and public benefits such as health care—the ACLU projects that taxpayers save $66,000 a year, on average, for each inmate over 50 our prisons set free. “States are confronting the complex, expensive repercussions of their sentencing practices,” notes a 2010 report from the Vera Institute for Justice.
It’s not difficult to see why it costs so much. “The medical conditions that present themselves to long-term elderly inmates run anywhere from dialysis to cardiac treatment to dementia,” says Carl ToersBijns, who worked his way up from guard to deputy warden during his 30 years in the New Mexico and Arizona prison systems. “It is staff intensive,” he says. And the number of elderly inmates “is outgrowing the ability of corrections officers to handle and manage them—they’re not medically trained.”
Nor are prison facilities designed for people with mobility problems. Their assisted-living and hospice units are often chock full, Hood says, leaving the unlucky elders stuck in the general population without the services they need. Unless states start releasing them, Hood says, we will need to “retrofit every prison in America to put assisted living-units in it, wheelchair accessibility, handicapped toilets, grab bars—the whole nine yards.”
 Kentucky inmate Charles Webb, 74, in 2008. Click above for more photos.
Kentucky inmate Charles Webb, 74, in 2008. Click above for more photos.
In recent months, I have been corresponding with several older men in Massachusetts state prisons, and have visited one of them in person. They are all lifers with murder convictions, which makes them atypical even among the long-termers. These men will never be paroled, and they are unlikely to qualify for early release no matter how rehabilitated they might be or how aged and decrepit they become. They have accepted this, and have generally tried to make something of their lives in prison—serving as jailhouse lawyers, organizing against abusive conditions, and helping their friends survive.
I am 75, so we share a camaraderie of sorts as we compare notes on our aches and pains and medication regimens. They know I understand what it’s like to be getting old and facing illness and death. They also know I have no idea what it’s like to deal with these things behind bars. Their letters tell of lives filled with daily indignities—trying to heave an aging body into the top bunk, struggling to move fast enough to get a food tray filled or get a book at the library, fighting off younger troublemakers. But worst of all is the pervasive nothingness and isolation.
Prison officials tend to discourage close friendships, and they dislike anything that smacks of organizing, which is considered a security threat. So they routinely transfer inmates between prisons and deny them the right to communicate with friends in other facilities. The activities available—which are few, since lawmakers wiped out most rehabilitative programming during the 1980s and 1990s—are accessible only to inmates who can walk long prison hallways or climb stairs. For some old-timers, a cell is their entire world; doing time simply means awaiting death.
Joe Labriola is a former Marine combat hero. Now 66, he joined the Marines at 17 and served two tours in Vietnam, receiving a Purple Heart and Bronze Star with Combat “V” for valor. After returning home, he was convicted of killing a drug dealer who was an FBI informant and got life without parole. So far he has served 38 years—18 in solitary.
Labriola has chronic breathing problems that he attributes to Agent Orange exposure. He says it’s hard to for him walk more than 10 steps without help from an oxygen machine, so he’s in a wheelchair a lot of the time. At least 75 prisons in 40 states now have hospices, but you won’t find any in Massachusetts. At MCI Shirley, Labriola lives in a ward called Assisted Daily Living, which he describes in his letters as a clutch of hospital beds in a corridor. “We live in an 11-man ward with all the beds side by side,” he says. “No ventilation or windows that can open. We do have hospital beds and standing wall lockers, something the general population does not have.” Unlike most assisted-living facilities, this setup provides little actual assistance, he says, other than what “the prisoners who clean the floor and bathrooms render us when we ask.” Residents get to move around outside the ward for just 10 minutes every hour, which means the person pushing Joe’s wheelchair must race from place to place—the prison library, he estimates, is a quarter mile away.
From his window, Labriola has a view of the prison hospital. “I see men coming up for medication and insulin at least three to four times per day,” he says. “They come in chairs, Canadian canes, geriatric walkers. In one week alone we had three deaths.” The hospital’s inpatient facilities consist of a series of five small wards with five beds in each. Men in various stages of bad health or terminal illness lie in bed all day long with nothing to do but watch soap operas. “What they need is mental, spiritual, and human stimulation in the form of a one-to-one care provided by trained prisoners who would be first cleared for drug usage and sex crimes as there are female nurses in the area,” Labriola suggests in one of his letters. “There are many men willing to volunteer their time and energies into making this a reality.”
Lifer John Feroli told the following story in one of his letters: “A guy in his 70s I knew personally was in the [solitary confinement] unit because he failed to stand for the afternoon count. He was on the third floor of the housing unit, he was partially paralyzed from a stroke and the batteries in his hearing aid were dead and he never heard the announcement for Count Time.”
Another convicted murderer, 73-year-old Billy Barnoski, wrote me in April to report that he was in solitary after a younger cellmate jumped him and beat him up. His friends came to his aid, there was a melee, and four people were thrown in the hole. Barnoski suffers from a heart condition called atrial fibrillation, which is treated with a blood thinner called coumadin. He also has high blood pressure, high cholesterol, shingles, and severe arthritis in his back and neck. He takes 25 pills daily. “There have been many times, so many, that they simply say, ‘We haven’t got that med today,'” he writes. “Mind you it has been heart meds just last week. Locked in this hole without necessary meds is torture.”
Then there’s Frank Soffen, also 73. Sentenced to life for second-degree murder, he has spent more than half of his life in prison. Nowadays he is confined to a wheelchair. He has kidney and liver disease and has suffered four heart attacks. He currently stays in the assisted living wing of Massachusetts’ Norfolk prison. And because of his failing health and his clean record during 40 years behind bars—which included rescuing a guard being threatened by other prisoners—he has been held up as a candidate for compassionate release.
Soffen is physically incapable of committing a violent crime. He cannot even hold a pen, in fact, so I had to rely on the other prisoners’ accounts of his situation. They told me has already participated in prerelease and furlough programs, and has a supportive family and a place to live with his son. One member of the state parole board recommended his release. But the board has denied him parole twice—in 2006 and again in January 2011. He won’t be eligible for review for another five years—if he lives that long. These days he’s warehoused in a medical observation bubble, bedridden, clad in adult diapers, unable to wash.
Gordon Haas, 68, is in better health, but he too has been in prison the better part of four decades, ever since his 1975 conviction for murdering his wife and children. While inside, Haas earned a master’s degree from Boston University, but such opportunities are exceedingly rare nowadays. Ever since Willie Horton—the furloughed Massachusetts prisoner who went AWOL and committed murder only to become the bane of Michael Dukakis’ 1988 failed presidential run—Haas has witnessed the rollback of parole and the end of programs that once allowed inmates to work outside prison gates and further themselves on the inside.
This past May, I visited Haas at Norfolk Prison, about 45 minutes outside Boston. Norfolk was designed for 750 men and holds 1,500. Built in during the 1920s to mimic a college campus, its buildings look more like dormitories than cell blocks, if you ignore the razor wire.
Haas tells me his advocacy for prison reform has earned him the scrutiny of the prison’s Inner Perimeter Security force, an internal police unit. They read his letters, he says, and monitor his phone calls. So rather than make a formal media request, I simply go in as a regular visitor.
Once I pass through the metal detectors—presenting ID, taking off my shoes and showing the bottoms of my feet, the underside of my collar, and the inside of my waistband—I proceed across the campus into a large visiting room filled with rows of chairs. Prisoners and visitors may sit next to, but not opposite, one another. They must keep their feet flat on the floor at all times and their backs against the chair backs. Guards posted at stations at either end of the room roam about and escort visitors to the toilet. Prisoners are strip searched before they enter and after they leave.
Haas enters wearing a short-sleeve button down, pressed blue jeans, and thick glasses. With his neatly combed gray hair, he reminds me of an IBM executive on a visit to the factory floor. He is affable, and a keen storyteller. In addition to leading the Lifers Group, a collection of men unlikely to ever get out, Haas is chairman of the Store & Finance Committee of the Norfolk Inmate Council. He takes a big interest in Project Youth, which teaches younger prisoners to speak to students and youth groups about what led them to prison.
As of June, according to its own figures, the Massachusetts Department of Corrections had 11,679 inmates. About 19 percent of them were 50 or older and 6 percent were at least 60. Last year, Haas used the DOC’s figures to produce his own report, which notes that the 60-plus contingent is the fastest-growing demographic in the state’s prisons.
Haas says he has been urging the state to adopt a hospice program for more than 15 years. “Our contention is that since lifers will probably be in need of such care, we are a resource for others now,” he says. But “the DOC does not sanction prisoners helping other prisoners. There is one outlet, and that is prisoners can volunteer to take those who can go outside out for programs and fresh air, even those in wheelchairs. That is good, but it is all there is.”
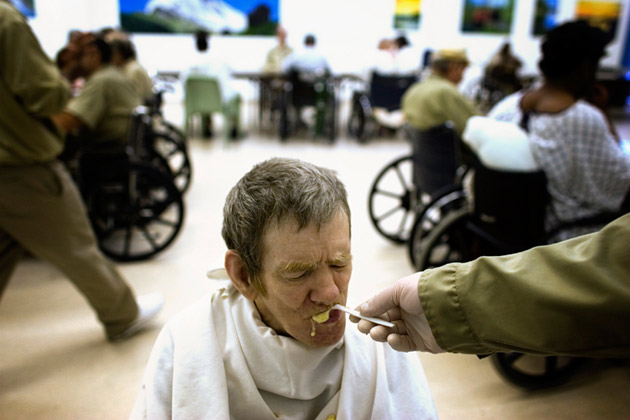 Lunch at Kentucky State Reformatory, 2008. Click above for more photos.
Lunch at Kentucky State Reformatory, 2008. Click above for more photos.
The DOC confirms that it has neither prison hospices nor immediate plans to build any. By 2020, according to the state’s DOC Master Plan, Massachusetts will need three “new specialized facilities” to house an estimated 1,270 prisoners with medical or mental health issues that would preclude them being housed in “regular” prisons. “We don’t have have a position on compassionate, geriatric, or any other type of release,” a DOC spokeswoman told me via email. “That’s up to the Legislature.” And while Massachusetts legislators have introduced a bill “establishing criteria for the compassionate release of terminally ill inmates,” it has yet to make it past the “study” stage.
By 2010, according to the Vera Institute, 15 states and DC had approved some form of “geriatric release,” while others had medical- or compassionate-release programs that could potentially apply to frail, aging prisoners. But “the jurisdictions are rarely using these provisions,” its report notes, thanks to fearful politicians, a less-than-sympathetic public, narrow eligibility criteria, and red tape that discourages inmates from applying and can draw out the process indefinitely. Nobody has aggregated the state-to-state data, but it appears that the number of prisoners released under these programs totals no more than a few hundred.
Jack Donson, who spent 23 years as a case manager for the federal Bureau of Prisons, points to the shortcomings of the Elderly Offender Pilot Program, part of 2008 federal legislation called the Second Chance Act. The law made the criteria for early release so strict, and the paperwork so extensive, Donson says, that it applied to only a few dozen inmates nationally. “I actually referred the first offender in the country” to the program, he notes on his website. “The bureaucrats deemed this offender dangerous to the community,” because of a record of violence 30 years earlier, “yet he had been incarcerated in a camp setting (without a fence), was a model inmate with an outstanding work ethic who even participated in unescorted medical furloughs in the community.”
Little has changed in the interim. But Hood believes America is approaching a politically expedient moment. “You spend $68,000 to watch an inmate who is truly hospital-bound? I think most people would get that. They would understand that if there’s another way to do it—let’s do it outside the prison,” he says. “Sixteen billion a year. Think about that number. It has to wake up some people.”
“States just can’t support the burden anymore,” agrees former state warden Carl ToersBijns. “The only solution will be to release them or to ignore them.” If we choose the latter, he cautions, prison death rates will skyrocket.
Of course, ignoring elderly prisoners after release could be just as devastating. The ACLU’s Fathi emphasizes that institutionalized old folks will require plenty of help transitioning back into the community and getting the services they need. “For many elderly prisoners,” he says, “particularly those with serious medical needs, simply pushing them out the prison door will be tantamount to a death sentence.”
James Ridgeway wrote this article with support from a MetLife Foundation Journalists in Aging Fellowship, a collaboration of New America Media and the Gerontological Society of America.















